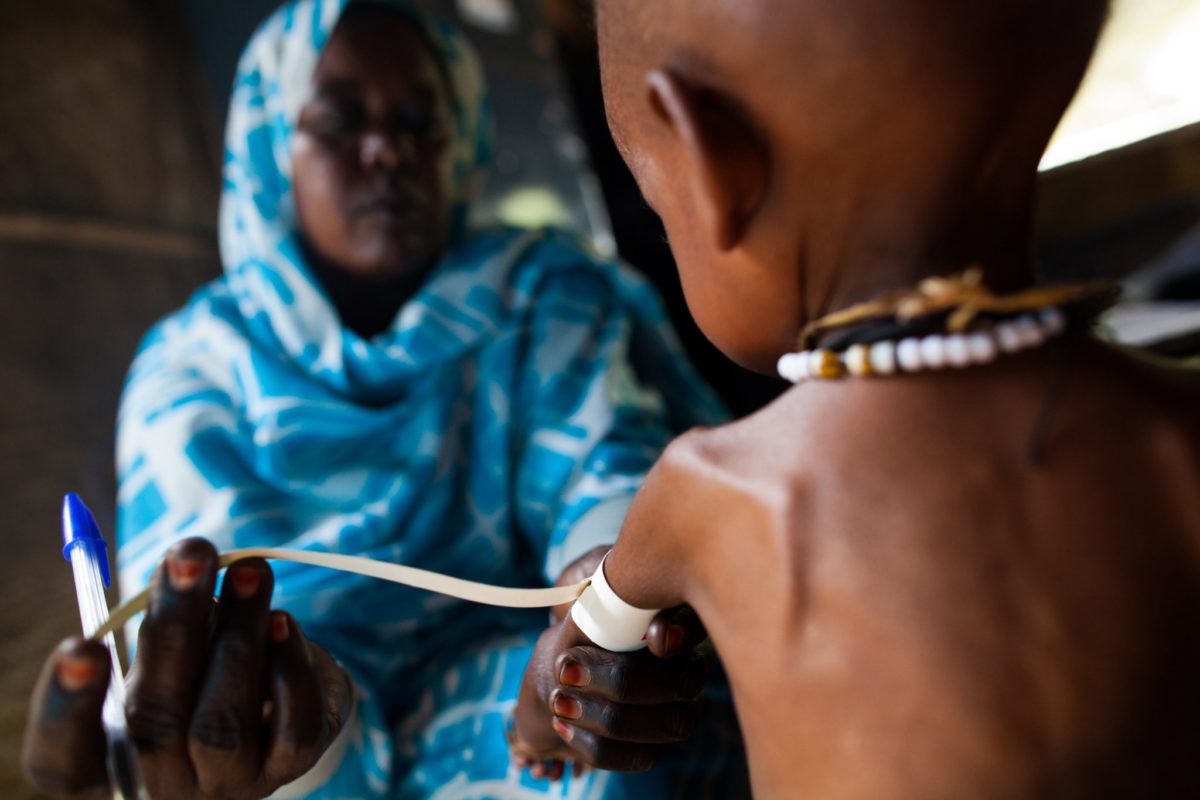
1,000 Days joins partners calling on global donors to fund nutrition crisis on World Food Day
This World Food Day, together with the International Rescue Committee and our partners we are calling on global donors to prioritize nutrition funding to combat the malnutrition crises. Malnutrition can be life-threatening for children, and rates are on the rise due to the impacts of COVID-19. There is no time to spare – donors and all stakeholders must step up now.
New York, NY, October 16, 2020 — The International Rescue Committee, together with CARE, 1,000 Days, HarvestPlus, Bread for the World, RESULTS Canada, KANCO, Concern Worldwide, Save the Children, World Vision, Action Against Hunger, and the Eleanor Crook Foundation endorse the following statement on World Food Day:
The Covid-19 pandemic, and its disruption to health and economic systems, is driving higher rates of a severe form of malnutrition. Urgent action is needed to save children’s lives and avert increased acute malnutrition and hunger during the pandemic and beyond. Global donors must increase their commitment to nutrition.
Year after year, over seven percent of the world’s children under age 5 – approximately 47 million children in 2019 – — suffer from a dangerous form of malnutrition referred to as acute malnutrition, or wasting. This form of malnutrition can increase mortality risk up to 11x that of a healthy child.
Covid-19 is driving rates of malnutrition up. World hunger is projected to rise to an additional 132 million people this year as a result of the pandemic, and acute malnutrition itself is projected to rise 14 percent– bringing the number of children under age 5 with acute malnutrition to 54 million. In four conflict-affected settings, the crisis is even more grave: Yemen, South Sudan, the Democratic Republic of Congo, and Northeast Nigeria are experiencing crisis-level food insecurity and acute malnutrition. The United Nations has recently warned that the situation in these countries is likely to worsen unless immediate action is taken. This stark increase in malnutrition, and the growing complexity of the hunger and nutrition landscape, threatens decades of progress to reduce child mortality.
Global progress on acute malnutrition has taken place slowly over the last twenty five years. Efforts to reach these children with life-saving treatment, called therapeutic foods, have been painfully slow, with only twenty percent of children needing treatment accessing it. Therapeutic foods were first developed in 1996, and yet remain widely unavailable to children in need. Prevention efforts like vitamin A supplementation and breastfeeding promotion must also be scaled up.
However, innovations in recent years have brought new hope for malnourished children.
New research into different approaches for treatment- including delivery by community health workers, and a simpler, more efficient treatment protocol- offer the promise of reaching more children, and stretching every dollar further. Recognizing the need for progress, last year United Nations Secretary General Antonio Guterres convened the leadership of United Nations agencies, and collectively they produced and agreed to an ambitious set of goals, released earlier this year as the Global Action Plan on Wasting. This commitment to accelerate progress- including scaling treatment to reach 50 percent more children- is paired with a commitment from the World Health Organization to review its guidelines on wasting, potentially paving the way for wider use of new approaches and innovations.
However, much remains to be done to reach the ambitious targets committed to in the Global Action Plan. United Nations agencies and national governments alike must maintain and increase resources for health systems- including investing in critical areas which are important for closing equity gaps and ensuring that every child can access the treatment they need.
Severe funding gaps
Despite the depth and severity of the needs, global nutrition efforts remain deeply underfunded. UN agency heads have indicated that $2.4 billion in additional investment is needed to truly protect children by preventing and treating acute malnutrition. This would support a full package of nutrition interventions- scaling up access to treatment, expanding prevention efforts like vitamin A supplementation, and promoting, protecting and supporting breastfeeding.
The most essential programming for nutrition response to the pandemic are outlined in the United Nations’ Global Humanitarian Response Plan. This plan has requested $247 million for essential nutrition response: to date, only three percent- approximately $7.7 million- has been funded.
Donors must commit to meeting the needs of these children
This World Food Day, we are calling attention to the deep, and increasing, need for nutrition funding. To avert increased child mortality due to increased acute malnutrition and hunger during the pandemic and beyond, global donors need to increase their commitment to nutrition.
Funding commitments to nutrition should be increased immediately through fulfillment of the UN’s Global Humanitarian Response Plan. And over the long-term, donors need to significantly increase long term funding commitments to nutrition: global donors should make strong commitments to address nutrition needs at next year’s Nutrition for Growth summit, including a doubling for nutrition-specific interventions like acute malnutrition treatment.
Covid-19 has stressed countries’ finances across the globe, but we cannot let millions more children suffer hunger, malnutrition, and even death, because of the pandemic.










 Damon ended up breached and I had a C-section. When I first came home from the hospital, I was so swollen from the anesthesia and other medications that I could not get off the couch without help, let alone take care of my brand new baby. I was already in so much pain because of my c-section, and on top of that I couldn’t walk because my legs were so swollen. Thankfully, my husband was able to get the first whole week off work. At the end of that week, still swollen and unable to care for Damon, I went to the hospital where they gave me medicine that reduced my swelling but made my breast milk dry up. If my husband could have stayed home a little longer, the swelling would probably have gone down on its own, and I could have breastfed my baby. Breastfeeding is healthier, cheaper and easier. I cried a lot after that, because I’m his mother and I’m supposed to provide that for him, and I couldn’t. But I didn’t have a choice.
Damon ended up breached and I had a C-section. When I first came home from the hospital, I was so swollen from the anesthesia and other medications that I could not get off the couch without help, let alone take care of my brand new baby. I was already in so much pain because of my c-section, and on top of that I couldn’t walk because my legs were so swollen. Thankfully, my husband was able to get the first whole week off work. At the end of that week, still swollen and unable to care for Damon, I went to the hospital where they gave me medicine that reduced my swelling but made my breast milk dry up. If my husband could have stayed home a little longer, the swelling would probably have gone down on its own, and I could have breastfed my baby. Breastfeeding is healthier, cheaper and easier. I cried a lot after that, because I’m his mother and I’m supposed to provide that for him, and I couldn’t. But I didn’t have a choice. I’m so thankful and blessed to have the ability to stay home with Damon now. Still, living paycheck to paycheck, not knowing if my husband’s income will be enough to cover the bills, is incredibly stressful. In an ideal world, paid leave would last at least three years, long enough for my child to have the ability to tell me about what’s going on in daycare. Without more paid leave, my options are to get a full-time job to relieve financial stress and put my baby in daycare where he could be harmed and can’t advocate for himself, or stay home and know he is well cared for but struggle to pay bills. Being a parent shouldn’t have to be like this.
I’m so thankful and blessed to have the ability to stay home with Damon now. Still, living paycheck to paycheck, not knowing if my husband’s income will be enough to cover the bills, is incredibly stressful. In an ideal world, paid leave would last at least three years, long enough for my child to have the ability to tell me about what’s going on in daycare. Without more paid leave, my options are to get a full-time job to relieve financial stress and put my baby in daycare where he could be harmed and can’t advocate for himself, or stay home and know he is well cared for but struggle to pay bills. Being a parent shouldn’t have to be like this.