CDC’s Grand Rounds on The Thousand Day Window
1,000 Days is honored to be a featured speaker at the CDC’s upcoming Grand Rounds to shine a spotlight on one of the biggest public health concerns facing our country: nutrition for moms and babies.
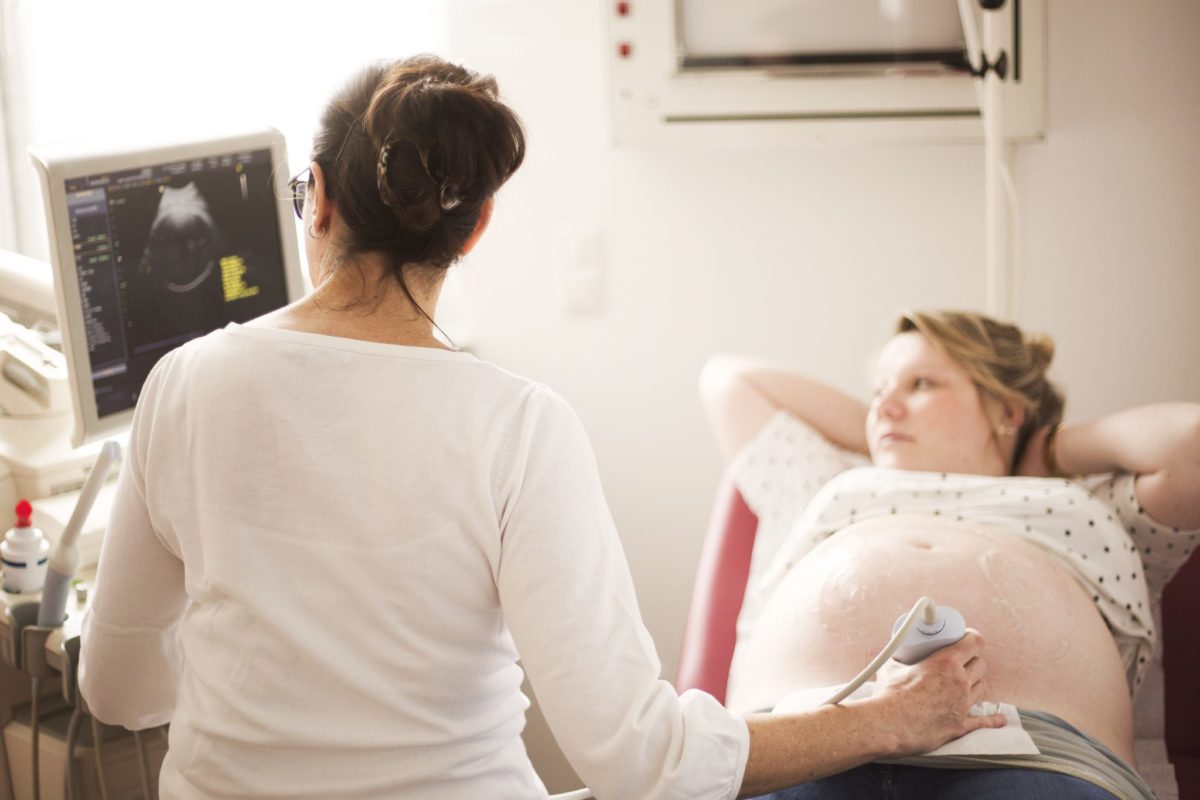
On Tuesday, June 18 from 1:00-2:00 pm EST, the U.S. Centers for Disease Control and Prevention (CDC) will present a Public Health Grand Rounds on “Maternal, Infant, and Early Childhood Nutrition—The Thousand Day Window of Opportunity.” One thousand days refers to the period from pregnancy through a child’s second birthday, when optimal nutrition is critical for brain development, healthy growth, and setting children on a trajectory for lifelong health.
During the Grand Rounds, an expert panel – led by Andrea Sharma an Epidemiologist with the Division of Nutrition, Physical Activity, and Obesity with the CDC, Michelle Kominiarek a physician with Northwestern University Feinberg School of Medicine, and Rafael Perez-Escamilla the Director of Yale School of Public Health – will explore how a woman’s nutrition during the first 1,000 days can impact both her own health and the child’s health, identify strategies that support women to breastfeed, and provide recommendations regarding an infant’s transition to the family diet. Together these factors have a profound impact on a child’s ability to grow, learn, and thrive.
Unfortunately, in the United States, optimal nutrition during the first 1000 days is not happening.
- About 16% of pregnant women have iron deficiency, with significant disparities by race/ethnicity.
- Almost 1 in 5 babies are never breastfed, and only 25% of infants are exclusively breastfed through 6 months.
- Among children 12-23 months, on a given day, fewer than half have eaten a vegetable and 1 in 3 consume a sugary drink.
- About 14% of U.S. children, aged 2-5 years, have obesity.
The CDC will use this key moment to uncover the science, statistics and research behind the state of the 1,000 days in the U.S. And they have invited 1,000 Days Executive Director Lucy Sullivan to be interviewed in a “Beyond the Data” segment that highlights the policies and practices impacting nutrition in the first 1,000 days and brings to light how these issues effect moms and babies.
Please join us for this live webcast to learn more about CDC’s role in Maternal, Infant and Early Childhood Nutrition.
We invite you to learn more about the state of the first 1,000 days in the U.S. View these resources to get started.












 1,000 Days calls for a comprehensive paid family and medical leave program that covers all workers. To best support families during the first 1,000 days, the program must:
1,000 Days calls for a comprehensive paid family and medical leave program that covers all workers. To best support families during the first 1,000 days, the program must: