Now more than ever, the political parties and candidates for office must focus on highly effective, science-based solutions to heal a sick country, and must make the difficult decisions to lift up the strategies with the highest return on investment. We have demonstrated that the best bet for investments that will show immediate impact, as well as future growth and prosperity, is one game-changing moment: the 1,000-day window.
The first 1,000 days between a woman’s pregnancy and a child’s 2nd birthday are a time of tremendous potential and enormous vulnerability. Research in the fields of neuroscience, biology and early childhood development provide powerful insights into how nutrition, relationships, and environments in this window shapes future outcomes. It is why several of the world’s leading economists have called for greater investments in the nutrition and well-being of mothers. With millions more people facing economic crisis as a result of the coronavirus pandemic, now is the time to ensure moms and babies have what they need to thrive – so that we all may thrive, too.
Specifically, we call on the candidates to include the following policies that:
- Strengthen and improve federal nutrition programs for all moms and babies who need them;
- Secure federal paid family and medical leave, enhancing millions of lives;
- Provide all moms and their young children access to quality, comprehensive health care;
- Create the environments for all moms to meet their breastfeeding goals; and
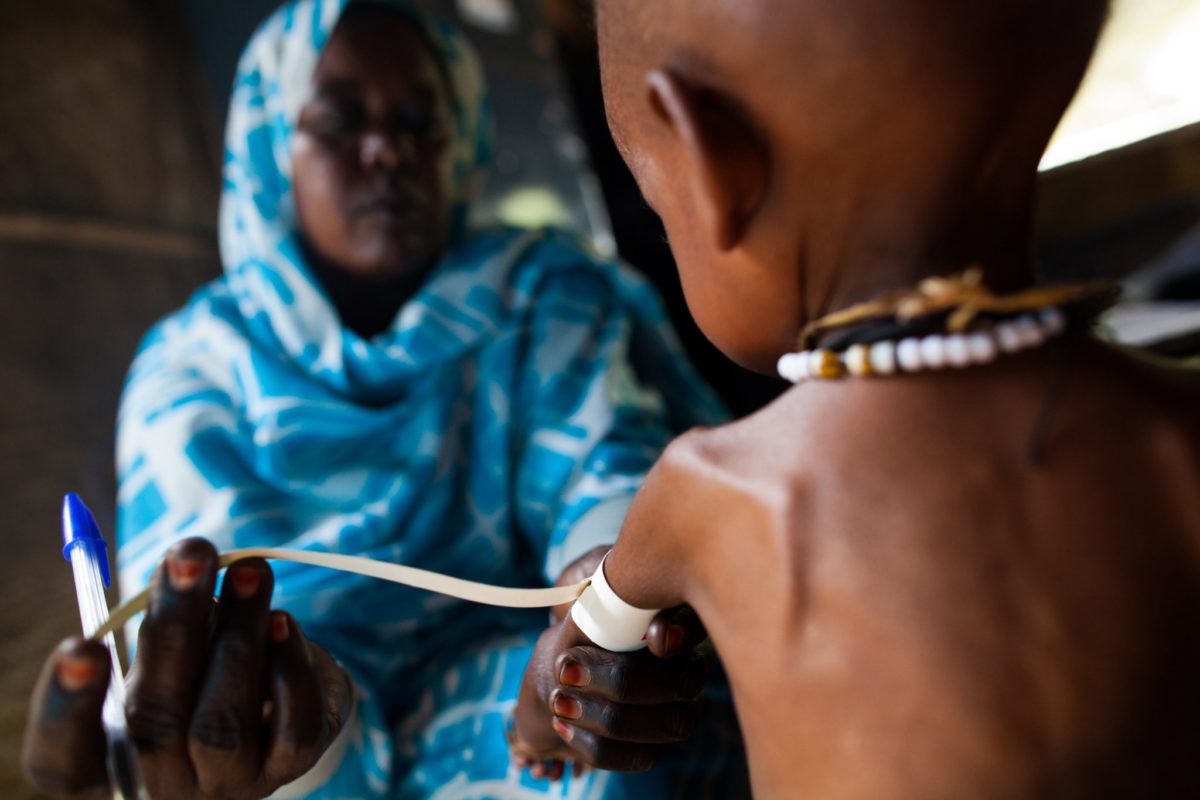
- Invest in the nutrition and well-being of mothers, infants and young children around the world, to curb severe malnutrition and avoid preventable child deaths.
The right investments, the right returns.
From India to Indiana, Kenya to Kentucky, mothers and children everywhere need good nutrition and nurturing care in the first 1,000 days in order to thrive.
Yet too many women and children in the U.S. and throughout the world do not get the food, health care or support they need during this pivotal moment that sets the foundation for all the days that follow. The consequences are often devastating. Globally, hundreds of millions of young children fail to reach their developmental potential, while millions more die every year as a result of malnutrition.
In the U.S., as in many other parts of the world, there are profound health disparities that contribute to unacceptably high maternal and infant mortality rates. And when we fail to nourish strong beginnings, we all feel the consequences—from persistent poverty and worsening inequality, to higher health care costs and weaker economies.
While the roots of malnutrition, disease, stunted development and inequality are often found in the first 1,000 days, so is the opportunity to build healthier and more equitable futures for children, women, their families and societies.
The time is now.
1,000 Days, Bread for the World and CARE, call on the candidates to include in the Party Platform the following policies and programs:
Invest in Federal Nutrition Programs
Too many moms and babies in the U.S. cannot access good nutrition. One out of six households with children under age 6 is food insecure, and one in five infants and toddlers under age 2 lives in poverty. Sadly, these numbers are on the rise as families struggle to cope with the economic fallout of the coronavirus pandemic, and families of color, low-income families, and single-parent households are particularly at risk. Federal nutrition programs play a critical role in helping all families get the nutrition and support they need to thrive, especially during times of hardship.
The Supplemental Nutrition Assistance Program (SNAP) provides nutrition assistance to help protect families against food insecurity. The Special Supplemental Nutrition Program for Women, Infants and Children (WIC) provides nutritious foods, nutrition education, breastfeeding support and health care referrals to low-income women who are pregnant or postpartum, infants and children under age 5. Investments in these programs must be protected and expanded to help ensure that all families in America can thrive.
Research shows that SNAP is effective in reducing food insecurity and leads to more regular access to food. It leads to improved birthweights, lower risks of developmental delays and better health, and it significantly reduces child poverty. Furthermore, the benefits of SNAP are long-lasting: when young children have access to SNAP, they have better health and improved economic self-sufficiency as adults.
WIC is one of the nation’s most successful and cost-effective nutrition intervention programs.
Research has shown that WIC reduces preterm and low birthweight births; reduces fetal and infant deaths; improves diet quality and nutrient status; increases access to prenatal care in early pregnancy; and saves health care costs.
The Party Platform must affirm its commitment to supporting and strengthening federal nutrition programs, including SNAP and WIC.
Support Paid Leave
The Policy Platform must include a comprehensive paid family and medical leave policy to support optimal child development, improve maternal health, reduce disparities, and enable future generations to live healthier lives.
Unlike in most other countries, in the U.S., parents are often unable to take time off from work to care for a new child, critically ill loved one, or tend to their own medical needs without sacrificing the income they need to support their families. This has profound and lasting impacts on maternal and child health in the United States. Because pregnancy, childbirth and the transition to motherhood can be physically and psychologically demanding, women need time to care for themselves and their health. Paid leave is a critical tool to support healthier pregnancies, better birth outcomes, more successful breastfeeding as well as both physical and mental health in the postpartum period. Additionally, inclusive and comprehensive policies can reduce the inequities in access to paid leave, helping to bridge the racial and ethnic disparities in overall maternal and child health outcomes.
Beyond allowing for physical recovery after childbirth, paid time off from work is essential to providing a strong foundation for mom, baby and their family to thrive. Science tells us that babies’ brains are nourished by time spent with parents and caregivers. Policies that enable parents to spend time nurturing and caring for their babies—particularly in the early weeks after birth and for babies that are born pre-term, low birth weight or with illness—are critical to the healthy cognitive, social, and emotional development of children.
For paid leave to have the kind of impact that will drive improvements to maternal and child health and child development, the policy must:
- Provide sufficient time off: Workers need access to a minimum of 12 weeks, but ideally 6 months (24 weeks), of paid leave annually to support the health and wellbeing of moms, children and their families.
- Cover all employers and all workers: Policies must be inclusive of all workers to ensure they can care for themselves or a loved one. Paid leave must be available to all workers regardless of the size of their employer, the sector they work in, the length of their employment or whether they work full-time, part-time or are self-employed.
- Ensure equitable economic security now and in the future: Workers should not have to decide between their health or caregiving responsibilities and their job. In addition, workers must retain the right to resume full paid employment after taking leave without fear of discrimination or retaliation. Policies must ensure that taking leave now does not threaten workers’ current or future economic security.
- Cover medical and family caregiving needs comprehensively: Any plan should be available for the full range of personal medical and family caregiving needs, such as those already established by the Family and Medical Leave Act (FMLA).
Support Pregnant and Postpartum Women in the Workforce
The Party Platform should include protections for pregnant workers and ensure that they cannot be discriminated or retaliated against for seeking appropriate accommodations.
The care and support a woman receives during her pregnancy has a profound impact on her health and on her child’s health. However, too many women—particularly low-income women and those who work in physically demanding occupations—are put in the impossible position of having to risk their health and their pregnancy in order to continue working so they can pay their bills and put food on the table. When workers are unable to receive necessary accommodations at work or are obligated to forgo their salary during pregnancy, the risk of pregnancy complications increases. Similarly, when pregnant women are pushed out of the workforce, their financial well-being and access to employer-provided health insurance and other benefits are compromised. This can have a long-term impact on a mother’s health and that of her child.
There is bipartisan support for protections for pregnant workers and we strongly encourage the Party Platform to include a national standard ensuring these protections.
Support Access to Quality, Comprehensive Health Care
The Party Platform should include the mandatory extension of Medicaid from 60-days to 1 year following the birth of a child and authorize coverage of services provided by lactation consultants to focus on the needs and concerns related to breastfeeding. Additionally, coverage must be comprehensive and not limited to pregnancy-related care. This will ensure that women can maintain their insurance and choice of health care providers in order to access their postpartum services.
The protections and support for women must extend beyond pregnancy as significant research has shown the lifelong impacts of co-morbidities during childbirth. Postpartum health care is an opportunity to assess a woman’s physical recovery from pregnancy and childbirth and to address: chronic health conditions, such as diabetes and hypertension; mental health status, including postpartum depression; and family planning. It is a time to provide support and services that she needs, including lactation support. In order for a child to thrive during their first 1,000 days, they need their mother to be supported in her recovery during this period, too.
Invest in Telehealth & Implicit Bias Training to Improve Maternal Health Crisis
The Party Platform must comprehensively address the maternal health crisis in America to reduce the number of pregnancy-related deaths among Black women. Too many Black women do not make it to the postpartum period and many more will never see the 1,000-day window as they are two to three times more likely to die from pregnancy-related causes than White women.
Unlike many other health disparities, Black maternal mortality cuts across zip codes impacting all socio-economic statuses. Studies have found that implicit bias is one of the main drivers of the unintentional deaths of which 60 percent are preventable, according to the CDC. Research shows that Black women receive a lower quality of care than White women and that they are treated differently even when they present with the same symptoms, receiving fewer diagnostic and therapeutic interventions and less pain medication, too, even following cesarean deliveries. In congruence with their peers, Black women should receive health care that is culturally competent and of the highest quality. Investments in implicit bias training for medical practitioners would help to identify and address this pervasive issue in health care, which would improve patient-provider interactions, health communication and, ultimately, health outcomes.
Additionally, investment in telehealth would reduce maternal mortality by expanding access to care in underserved areas with high rates of maternal mortality and severe maternal morbidity. Almost 65,000 Black women die from pregnancy- and childbirth-related causes each year. These near-misses have lifelong consequences for women’s health, resulting in higher utilization of health services, higher direct medical costs and the need for long-term rehabilitation, including mental health services. Telehealth could have a particular impact by expanding remote patient monitoring throughout a woman’s pregnancy and during the critical postpartum period.
Invest in Global Nutrition
The party platform should prioritize global nutrition as a key component of its global health strategy and increase funding for the nutrition sub-account within the global health account at USAID. Severe malnutrition is the number one killer of kids under age 5, killing more children every year than AIDS, Malaria, and Tuberculosis combined and afflicting many of those children who survive with lifelong illness and impaired cognitive development. Around the world, leading scientists and economists have consistently demonstrated that global nutrition interventions are some of the most successful, cost-effective, and scalable development investments, yielding up to $35 in economic returns for every $1 the U.S. spends.
Yet, despite these strong incentives, nutrition remains drastically underfunded, receiving less than 1% of official development assistance funding. Severe malnutrition stunts potential and wastes lives, but it does not have to. Scaling up proven nutrition interventions will allow children around the world to escape these preventable deaths.
Malnutrition has many root causes, including poverty, lack of education, erratic seasonal crop cycles, climate change, women’s inequality, and poor access to water, sanitation, and hygiene. As the world works to tackle these major challenges, which will help end child malnutrition in the long-term, there are four essential actions the U.S. can take now to prevent children from dying of severe malnutrition:
- Supply all pregnant women with prenatal vitamins, especially multiple-micronutrient supplements (MMS);
- Support breastfeeding mothers through one-to-one and group breastfeeding counseling;
- Continue bi-annual Vitamin A Supplementation, especially in conjunction with large-scale vaccination campaigns;
- Expand coverage of specialized foods for treatment including by prepositioning Ready-to-Use Therapeutic Food (RUTF) in vulnerable communities in anticipation of a dramatic rise in cases of wasting as a result of COVID-19.
The need is greater as we face a global pandemic.
Today, we are learning how COVID-19 disproportionately impacts women, girls and marginalized populations in the U.S. and around the world. Along with staggering mortality rates, the pandemic has led to soaring unemployment, giving rise to a new population at risk. Meanwhile, low-wage workers continue to serve their communities at the “new frontlines” of food service, home health aides, for example – putting themselves at risk without the guarantee of paid leave or health benefits.
In countries that offer more comprehensive support for families — like Germany, France, Canada and Sweden — a significantly larger proportion of women are in the labor force. Yet, in the United States, parents are often forced to choose between taking time off from work to care for their young children and earning the income they need to support their families. In fact, only a small minority of private sector workers in the U.S. — typically those who work in higher paid jobs — have access to paid leave. This means that many women return to work too soon after giving birth, putting their health and that of their infant at risk. Without a mandate for U.S. employers to offer paid leave, 81% of mothers receive no paid time off to care for their newborn child.
As the world focuses on the containment of COVID-19, urgent action is needed to avoid the long-term and large-scale impacts on malnutrition and preventable deaths from the secondary effects of this crisis. We have long understood that increased undernutrition compromises immune systems, making bodies vulnerable to virus attacks and impeding recovery. People living with pre-existing medical conditions, and suffering from non-communicable diseases (NCDs, such as obesity, heart disease, type 2 diabetes, and some cancers), appear to be more at risk of developing severe COVID-19 symptoms and have higher mortality rate than other populations.
The COVID-19 pandemic has yet to be reported at scale in some of the most impoverished parts of the world. Government leaders are beginning to sound the alarm on the fragility of health systems, food systems, and economies in many low- and middle-income countries, which already face high rates of severe malnutrition. COVID-19 will put vulnerable children and families at even greater risk of falling into the vicious intergenerational cycle of malnutrition, ill health, and poverty. For children in the first 1,000 days, even a short bout of malnutrition can have devastating lifelong consequences. The secondary consequences of this pandemic risk the lives and potential of an entire generation.
In the short term, employment uncertainty, closing of schools, closing of borders, periods of isolation, and widespread sickness has implications for millions of people vulnerable to food poverty. As governments are responding to this health crisis, multi-sectoral nutrition and food security programs must be safeguarded to protect children and families vulnerable to malnutrition. Not only do we want to prevent a protracted nutrition crisis, but nutrition itself will play a role in recovery to help increase immunity and resiliency.

 Damon ended up breached and I had a C-section. When I first came home from the hospital, I was so swollen from the anesthesia and other medications that I could not get off the couch without help, let alone take care of my brand new baby. I was already in so much pain because of my c-section, and on top of that I couldn’t walk because my legs were so swollen. Thankfully, my husband was able to get the first whole week off work. At the end of that week, still swollen and unable to care for Damon, I went to the hospital where they gave me medicine that reduced my swelling but made my breast milk dry up. If my husband could have stayed home a little longer, the swelling would probably have gone down on its own, and I could have breastfed my baby. Breastfeeding is healthier, cheaper and easier. I cried a lot after that, because I’m his mother and I’m supposed to provide that for him, and I couldn’t. But I didn’t have a choice.
Damon ended up breached and I had a C-section. When I first came home from the hospital, I was so swollen from the anesthesia and other medications that I could not get off the couch without help, let alone take care of my brand new baby. I was already in so much pain because of my c-section, and on top of that I couldn’t walk because my legs were so swollen. Thankfully, my husband was able to get the first whole week off work. At the end of that week, still swollen and unable to care for Damon, I went to the hospital where they gave me medicine that reduced my swelling but made my breast milk dry up. If my husband could have stayed home a little longer, the swelling would probably have gone down on its own, and I could have breastfed my baby. Breastfeeding is healthier, cheaper and easier. I cried a lot after that, because I’m his mother and I’m supposed to provide that for him, and I couldn’t. But I didn’t have a choice. I’m so thankful and blessed to have the ability to stay home with Damon now. Still, living paycheck to paycheck, not knowing if my husband’s income will be enough to cover the bills, is incredibly stressful. In an ideal world, paid leave would last at least three years, long enough for my child to have the ability to tell me about what’s going on in daycare. Without more paid leave, my options are to get a full-time job to relieve financial stress and put my baby in daycare where he could be harmed and can’t advocate for himself, or stay home and know he is well cared for but struggle to pay bills. Being a parent shouldn’t have to be like this.
I’m so thankful and blessed to have the ability to stay home with Damon now. Still, living paycheck to paycheck, not knowing if my husband’s income will be enough to cover the bills, is incredibly stressful. In an ideal world, paid leave would last at least three years, long enough for my child to have the ability to tell me about what’s going on in daycare. Without more paid leave, my options are to get a full-time job to relieve financial stress and put my baby in daycare where he could be harmed and can’t advocate for himself, or stay home and know he is well cared for but struggle to pay bills. Being a parent shouldn’t have to be like this.